

Glaucoma is a potentially blinding eye disease characterized by an abnormal buildup of fluid pressure within the eye. Under normal conditions the fluid produced within the eye leaves the eye through a drainage canal system.
Eventually the fluid returns to the bloodstream. When the production of the fluid is more than the drainage, the pressure within the eye increases.
As the pressure increases, damage can occur to the optic nerve. Most patients develop glaucoma because of poor drainage of fluid through the drainage canal.
The problem works like a plumbing problem when water backs up because of clogged pipes. This increased pressure in the eye results in nerve damage and irreversible loss of vision including potential blindness.
Glaucoma is the leading preventable cause of blindness in the United States. Currently about 2 million Americans are being treated for glaucoma. An equal number of people suffer from undiagnosed cases. In its early stages, this disease is without symptoms. It gradually and painlessly “sneaks up” and attacks over a period of time. If left undetected and untreated, glaucoma can leave its victims blind. Once vision is lost to glaucoma, it cannot be restored. About one out of every 50 adults develops glaucoma; however, the risk of developing it dramatically increases after age 40. For certain high risk groups regular glaucoma checkups are very important:
We know what glaucoma is and does, but we still do not know what causes it despite extensive research.
To understand how glaucoma develops, we must first understand the delicate and sophisticated mechanism of the eye.
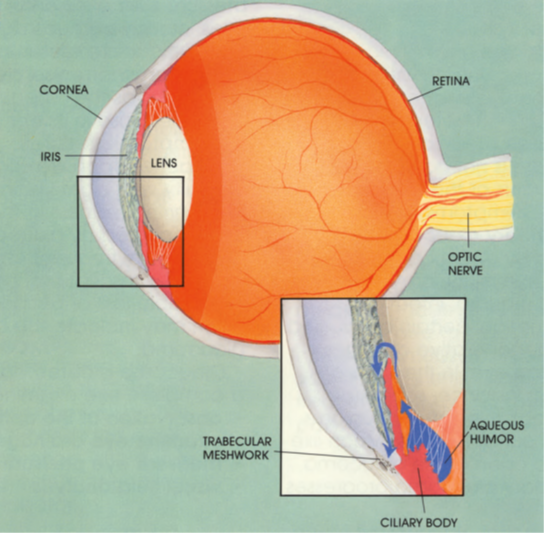
The eye functions like a camera. In the front is the cornea, a transparent tissue which protects and allows light to enter, much like a window. The colored part of the eye, the iris, is directly behind the cornea. It opens and closes like a camera shutter to control the amount of light which enters the eye. Within the iris is the pupil, the small black-looking opening which continues to admit the correct amount of light. The lens then focuses that light on the retina, which, like film, records the light images. The retina sends visual messages to the brain via the optic nerve.
The front part of the eye, the anterior and posterior chambers, is filled with a fluid called aqueous humor. This fluid maintains normal pressure inside the eyeball, preventing it from collapsing ––like a balloon filled with air. The fluid is constantly produced by the ciliary body and drains back to the bloodstream through the trabecular meshwork. Blockage or overproduction of the fluid elevates pressure (intraocular pressure) within the eyeball.
Abnormally high pressure for an extended period of time in eyes with glaucoma creates damage to the optic nerve and loss of vision.
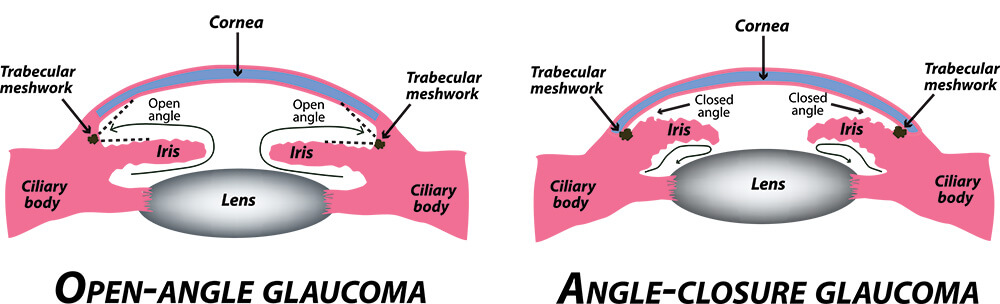
Ninety percent of all glaucoma cases are of the chronic open angle or normal pressure variety. In this type, the drainage system functions incorrectly, resulting in a gradual pressure rise over time. As this pressure increases, the optic nerve is damaged, and side (or peripheral) vision begins to deteriorate. Ocular hypertension is a very common condition in which the pressure within the eye elevates, but the optic nerve and peripheral vision shows as normal. This condition progresses in some cases to open angle glaucoma.
A less common yet more alarming type is narrow or acute angle closure glaucoma. This version strikes suddenly and severely in the form of blurred vision, headaches, severe pain, nausea, or rainbows around lights. With acute glaucoma there is a sudden increased pressure within the eye caused by a mechanical blockage of the drainage angle (trabecular meshwork). Unfortunately, permanent damage including blindness can potentially occur if immediate medical emergency treatment is not administered within hours of the appearance of these symptoms.
Secondary glaucoma can be caused by a number of factors like an eye injury, previous eye surgery, trauma, infection, inflammation, certain drugs, and other degenerative changes within the eye. In the case of injury for instance, scar tissue can block the natural passage of fluid out of the eye. Much like chronic open angle glaucoma, secondary glaucoma progresses over time.
Congenital glaucoma is found in infants and is very rare. The fluid drainage area is abnormal at birth and must be surgically treated as soon as possible to save the infant’s vision. Since infants have a more elastic eye than adults, the increased pressure will cause enlarged eyes, cloudy corneas, light sensitivity, and excessive tearing. Glaucoma is frequently referred to as the “sneak thief of sight” because in its early stages it is symptomless. Later, headaches upon waking, difficulty with night vision, reoccurring redness in the eye(s)accompanied by blurred vision and or pain, frequent changes in eyeglass prescriptions, or noticeable loss of peripheral vision may indicate the onset of glaucoma.
Glaucoma is detected through a complete eye examination:
The examination and evaluation for glaucoma include the use of specially designed instruments.
Observation of the drainage angle is performed by using a gonioscope, a specially mirrored and magnified lens that functions like a periscope.
The lens magnifies and bends light to allow observation of the structures of the trabecular meshwork.
Tonometry measures the pressure within the eye in millimeters of mercury.
The cornea (front of the eye) is gently touched with a very sensitive instrument called an applanator.

The evaluation of the optic nerve to locate characteristic nerve damage is performed with this instrument.
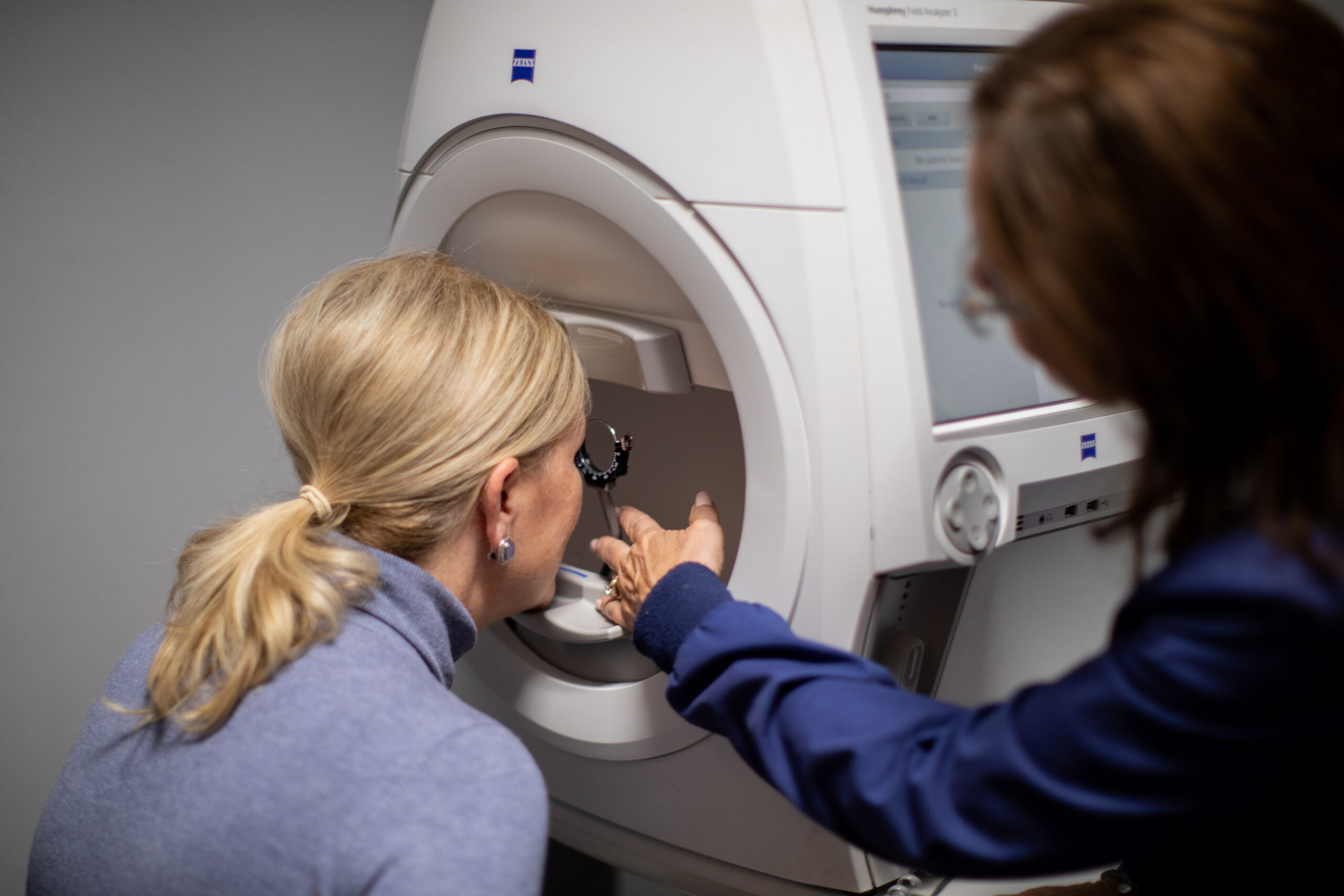
Visual field testing detects and measures the severity of the vision loss due to glaucoma.
This instrument measures the loss of side or peripheral vision, which frequently occurs without the patient’s knowledge.
This test uses light waves to take cross-section pictures of your optic nerve and macula. This allows us to see evaluate the nerve fiber layer and cells of your macula (ganglion cells). These measurement’s help with diagnosis of glaucoma and allow us to track one’s stability over time.

This test measures the thickness of the cornea. Checking the intraocular pressure by tonometry assumes a normal corneal thickness.
If the cornea is too thick or too thin there is an adjustment made in the intraocular pressure based on the pachymetry reading.
